Breast Reconstruction After Mastectomy
Overview
Breast reconstruction after mastectomy is a surgical process that may be performed to recreate a breast mound following breast removal, which is commonly part of breast cancer management or risk-reduction surgery. Reconstruction planning is individualised and considers factors such as your anatomy, the type of mastectomy, overall health, and any current or planned cancer treatments (including radiotherapy). A consultation is required to discuss suitability, the stages of reconstruction, expected outcomes and limitations, risks, scarring, recovery, and alternatives.
Add volume to breasts
Reduce sagging
Lift and tighten
Reshape and contour
Before & After
The outcomes shown are only relevant for this patient and do not necessarily reflect the results other patients may experience, as results may vary due to many factors including the individual’s genetics, diet and exercise.
Breast Augmentation
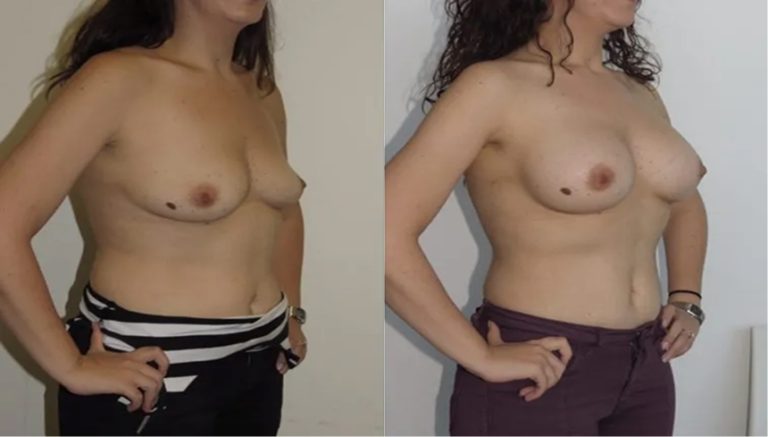
Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation
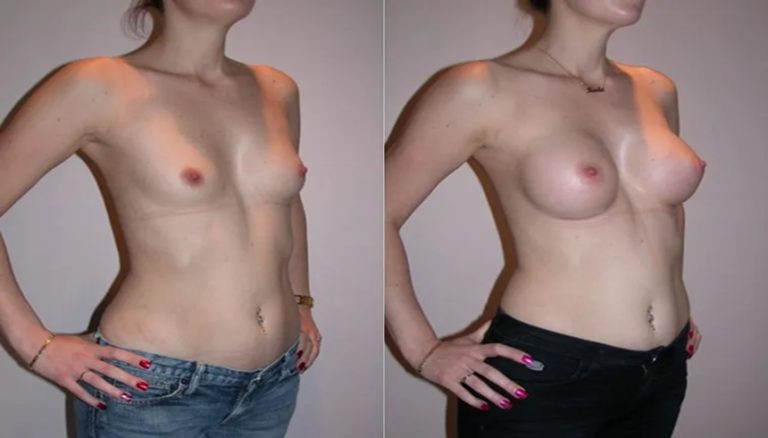
Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
About This Procedure
Breast reconstruction after mastectomy may involve rebuilding the breast using:
- Implants, or
- Your own tissue (autologous reconstruction / flap surgery), or
- A combination of both approaches.
Reconstruction may be performed at the time of mastectomy (immediate reconstruction) or at a later date (delayed reconstruction). Some people have reconstruction in multiple stages. The aim is to create a breast shape that is appropriate for the individual and the clinical context. Symmetry cannot be guaranteed, and additional procedures may be recommended to refine contour or address balance between sides.
Your Consultation with Dr Lajevardi
Dr Sepehr Lajevardi is a highly skilled and experienced plastic surgeon, dedicated to providing exceptional results to each patient. He takes a caring approach, working with patients to create an individualised treatment plan that helps them feel confident in their outcomes. Book your appointment to receive professional care and guidance from Dr Lajevardi, and find out if breast augmentation surgery is right for you.

Key Benefits
Recreating a breast mound
Reducing reliance on external prostheses
Clothing fit considerations
Staged reconstruction options
Complete Breast Guide
Get step-by-step insights, recovery tips, and expert recommendations for your Breast. Download our free guide today.
Ideal Candidate
You May Be a Good Candidate If
You may be a good candidate for breast reconstruction if you:
- Are in good overall physical health (as assessed clinically)
- Have discussed reconstruction timing with your treating team (e.g., breast surgeon/oncology team)
- Have realistic expectations about variability in outcomes, scarring, and the possibility of staged procedures
- Do not smoke or are willing to stop nicotine use for a specified period before and after surgery (as directed)
- Have anatomy that supports the planned reconstruction method (for example, adequate donor tissue for a flap, or suitability for an implant-based approach)
Who Should Not Undergo This Procedure
Reconstruction may be unsuitable or higher risk for individuals who:
- Have uncontrolled medical conditions that increase surgical risk
- Have an active infection
- Are unable to stop nicotine use where clinically required
- Have factors that significantly increase healing risks (for example, compromised blood supply to the chest area)
- Have unrealistic expectations regarding symmetry, scarring, or the number of stages required
Surgical Techniques & Approaches
Implant-Based Reconstruction:
This approach uses an implant to create the breast mound. It may be performed as:
- A two-stage process with a tissue expander followed by exchange to a permanent implant, or
- A single-stage approach in selected cases, depending on clinical factors.
Your surgeon will explain implant options, the likely number of stages, and implant-related risks. Implants are not lifetime devices and may require future surgery.
Tissue-Based (Flap) Reconstruction:
This approach uses your own tissue (skin and fat, and sometimes muscle) from another part of the body. Common donor sites include the abdomen, back, or buttock region. Examples of flap techniques include DIEP flap and latissimus dorsi flap, among others.
Flap procedures are complex operations and involve scarring at both the breast and donor site. Suitability depends on anatomy and medical factors, and not every patient is a candidate for every flap type.
Your surgeon will explain recommended options, incision planning, scarring expectations, and the trade-offs of each approach.
Anesthesia
Breast reconstruction is commonly performed under general anaesthesia. The anaesthesia plan depends on the type and extent of reconstruction, patient factors, and the operating facility’s protocols and will be discussed during consultation.
Pre-Operative Preparation
Preparation typically includes:
- Medical review: including medications, supplements, and relevant investigations (where required).
- Medication guidance: you may be asked to stop certain medications/supplements that can increase bleeding risk (where clinically appropriate).
- Nicotine cessation: nicotine can impair healing; you may be asked to stop smoking/vaping/nicotine products for a specified period before and after surgery.
- Fasting instructions: follow the facility’s requirements prior to anaesthesia.
- Support planning: arrange transport and post-operative support after discharge.
Recovery Process
Timeline
Activity & Expectations
Immediately Post-Op
Weeks 2–4
Ongoing changes in swelling, contour and scar healing occur. Return to exercise is guided by clinical review and depends on donor site healing (if applicable).
Scars continue to mature. Breast shape and contour can continue to evolve. Timelines vary, particularly when reconstruction is staged.
Recovery Milestones
Return to Work
Return to Exercise
Appearance over time
Resources & Guides
A breast augmentation is a very customized procedure, and selecting an experienced surgeon is paramount. Dr. Lajevardi focuses on patient safety, naturally appearing results, and transparency throughout the process.
Patient Preparation Guide
Procedure Walkthroughs

Procedure Walkthroughs

Patient Preparation Guide
Frequently Asked Questions
Procedure & Results
How long does Breast Reconstruction surgery take?
Will I have noticeable scars?
How long will the results last?
Longevity varies. Autologous (tissue-based) reconstruction changes over time with the body. Implant-based reconstruction may require additional surgery in the future because implants are not lifetime devices. Ageing, weight changes, and cancer treatments such as radiotherapy can influence long-term appearance.
What are the risks associated with Breast Reconstruction?
Risks include bleeding, infection, scarring, delayed wound healing, seroma, changes in sensation, and anaesthetic risks. Implant-related risks include capsular contracture, rupture/deflation, and malposition. Flap-related risks include partial or total flap compromise, donor site complications, and longer recovery. A detailed discussion of risks and alternatives will occur during consultation.

