Tuberous Breast Correction
Tuberous Breast Correction (Congenital Breast Development Differences) in Sydney
Overview
Tuberous breast correction is a specialised surgical procedure that may be considered for people with tuberous (tubular) breast development, a congenital variation where breast shape and base width may develop differently. Surgical planning is individualised and may involve releasing constricting tissue at the breast base and reshaping breast tissue. Some cases may also involve implants and/or fat grafting, depending on anatomy and the treatment plan. A consultation is required to assess suitability and to discuss expected changes, limitations, risks, scarring, recovery, and alternatives.
Add volume to breasts
Reduce sagging
Lift and tighten
Reshape and contour
Why Consider Breast Augmentation?
- Numerous women select breast augmentation to
- Enlarge naturally small breasts
- Re-establish lost volume post-pregnancy or weight gain
- Refine asymmetry for a better-balanced look
- Re-create a more youthful, full contour
While outcomes are not the same, the procedure can yield long-lasting enhancements in looks and confidence. But keep realistic expectations in mind—individual results are based on body type, implant choice, and healing.
Add volume to breasts
Reduce sagging
Lift and tighten
Reshape and contour
Before & After
The outcomes shown are only relevant for this patient and do not necessarily reflect the results other patients may experience, as results may vary due to many factors including the individual’s genetics, diet and exercise.
Breast Augmentation
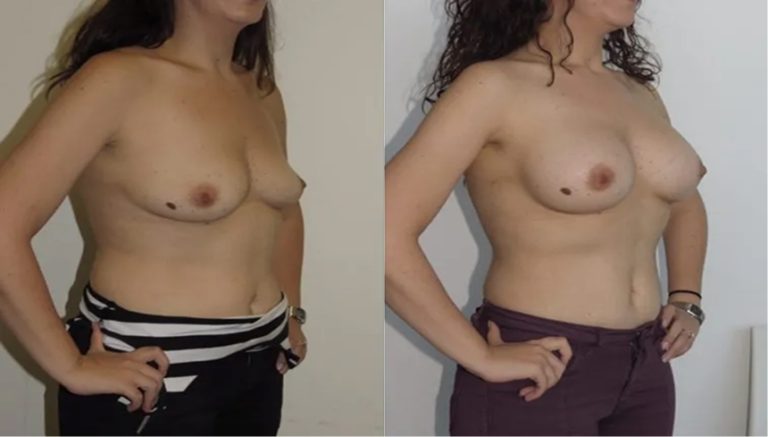
Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation
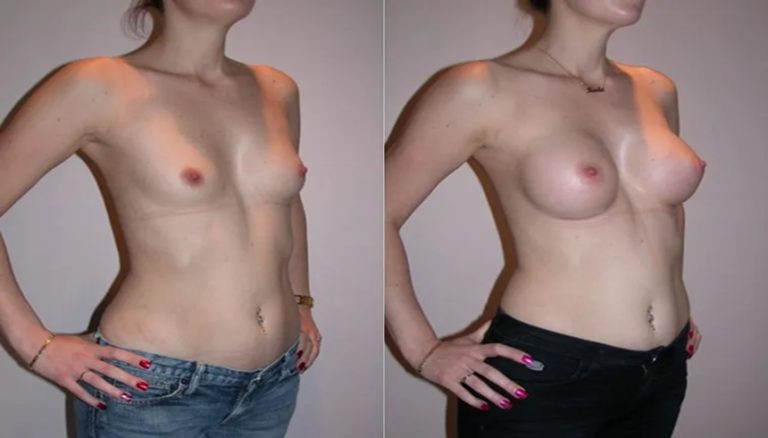
Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
About This Procedure
Tuberous breast correction addresses structural features that can be seen in tuberous breast development, which may include:
- A constricted breast base (narrow base width)
- Limited development of the lower breast pole
- Herniation of breast tissue into the areola in some cases
- Asymmetry between breasts
The procedure is tailored to the individual and may involve reshaping or redistributing breast tissue, with or without volume augmentation. All surgical procedures result in scars, and scar appearance varies between individuals.
Your Consultation with Dr Lajevardi
Dr Sepehr Lajevardi is a highly skilled and experienced plastic surgeon, dedicated to providing exceptional results to each patient. He takes a caring approach, working with patients to create an individualised treatment plan that helps them feel confident in their outcomes. Book your appointment to receive professional care and guidance from Dr Lajevardi, and find out if breast augmentation surgery is right for you.

Key Benefits
The aim of tuberous breast correction is to address the anatomical features associated with tuberous breast development. Depending on individual anatomy and the surgical plan, potential physical changes may include:
Change in breast base width and contour
release and reshaping may allow a broader breast base and altered breast mound shape.
Change in lower-pole fullness
tissue rearrangement may improve lower-pole shape in some cases.
Change in areola appearance
areolar size and/or protrusion may be modified where clinically appropriate.
Change in symmetry
Outcomes vary and depend on the degree of tuberous development, tissue characteristics, healing, and whether implants or fat grafting are used.
Complete Breast Guide
Get step-by-step insights, recovery tips, and expert recommendations for your Breast. Download our free guide today.
Ideal Candidate
A suitable candidate is generally a physically healthy adult with features consistent with tuberous breast development, who understands that outcomes and scarring vary and that additional procedures may be required in some cases. A consultation is needed to confirm diagnosis, assess anatomy, and discuss the surgical plan, recovery, and risks.
You May Be a Good Candidate If
You may be a good candidate for tuberous breast correction if you:
- Are in good overall physical health
- Have features consistent with tuberous/tubular breast development
- Would like an assessment for breast reshaping and/or volume options
- Have realistic expectations about variability in outcomes and recovery
- Do not smoke or are willing to stop nicotine use for a specified period before and after surgery (as directed)
- Have completed breast development (commonly late teens/early adulthood—individual variation applies)
Who Should Not Undergo This Procedure
Tuberous breast correction may not be suitable for individuals who:
- Have an active infection
- Are currently pregnant or breastfeeding
- Have uncontrolled medical conditions that increase surgical risk
- Are unable to stop nicotine use where clinically required
- Have significant weight instability where timing may affect planning and healing
- Have unrealistic expectations about outcomes
Surgical Techniques & Approaches
There is no single approach that suits everyone. The technique is determined by anatomy, the degree of tuberous development, skin quality, and the agreed treatment plan. Options may include:
Release of constricting tissue:
to expand the breast base and allow reshaping.
Glandular tissue redistribution:
to reposition tissue into areas where development is limited (often the lower pole).
Areolar adjustment (where appropriate):
to address areolar size and/or protrusion.
Volume augmentation (case-by-case):
some patients may require implants and/or structural fat grafting to support shape or volume distribution.
Your surgeon will explain incision options, scar placement, trade-offs, and why a particular approach is recommended for your anatomy.
Anesthesia
This procedure is commonly performed under general anaesthesia. The anaesthesia plan depends on the procedure extent, patient factors, and the operating facility’s protocols and will be discussed during consultation.
Pre-Operative Preparation
- Medical review: history, medications, supplements, and relevant investigations (where required).
- Medication guidance: you may be asked to stop certain medications/supplements that can increase bleeding risk (where clinically appropriate).
- Nicotine cessation: nicotine can impair healing; you may be asked to stop smoking/vaping/nicotine products for a specified period before and after surgery.
- Alcohol guidance: you may be advised to limit alcohol before surgery.
- Fasting instructions: follow the facility’s instructions prior to anaesthesia.
- Support planning: arrange transport and post-operative support, especially if general anaesthesia is used.
Recovery Process
Timeline
Activity & Expectations
Immediately Post-Op
You may wake with dressings and a support bra/garment if advised. Monitoring occurs in recovery. Drowsiness, nausea, tightness and discomfort can occur.
First 24–48 Hours
Rest is commonly recommended. Discomfort varies and is managed according to your clinician’s plan. Swelling and bruising are common early.
Week 1
Follow-up is usually scheduled. Activity restrictions commonly include avoiding lifting, stretching, and heavy arm/chest movement.
Swelling and bruising often reduce gradually. Return to light work may be possible depending on role and healing. Support garments may be advised.
Ongoing changes in swelling and breast shape can occur. Activity is increased gradually based on clinical review.
Scars continue to mature. Final appearance can continue to evolve for many months and varies between individuals.
Recovery Milestones
Return to Work
Timing varies depending on the extent of surgery, healing, and the physical demands of your job.
Return to Exercise
Light activity may be resumed as advised. Strenuous exercise and heavy lifting are typically restricted for a period determined by your surgeon.
Appearance over time
Breast shape can continue to change during healing. If implants are used, implant position can evolve over time. There is no single timeline that applies to everyone.
Resources & Guides
A breast augmentation is a very customized procedure, and selecting an experienced surgeon is paramount. Dr. Lajevardi focuses on patient safety, naturally appearing results, and transparency throughout the process.
Patient Preparation Guide
Procedure Walkthroughs

Procedure Walkthroughs

Patient Preparation Guide
Frequently Asked Questions
Procedure & Results
How long does the Tuberous Breast Correction surgery take?
Timing varies depending on the degree of tuberous development and the techniques used (for example, tissue reshaping, implants, and/or fat grafting). Your surgeon will provide an estimate after assessment.
Will I have noticeable scars?
All surgery results in scars. Incision placement depends on the surgical plan and may include periareolar incisions and/or additional incisions depending on technique. Scar visibility varies based on individual healing and aftercare.
How long will the results last?
Longevity varies. Ageing, pregnancy, weight changes, and gravity can affect breast appearance over time. If implants are used, they are not lifetime devices and may require additional surgery in the future.
What are the risks associated with Tuberous Breast Correction?
Risks include bleeding, infection, scarring, delayed healing, asymmetry, changes in nipple/breast sensation, and the possibility of revision surgery. If implants are used, risks can include capsular contracture, rupture/deflation, and implant malposition. Anaesthetic risks also apply. A detailed discussion of risks and alternatives will occur during consultation.
Pain & Recovery
Is the Tuberous Breast Correction procedure painful?
Discomfort varies. Many people experience tightness or soreness in the early recovery period. Pain management options and aftercare instructions will be provided.
What kind of pain medication will I be given?
Medication plans vary and depend on individual factors and clinical judgment. Your surgeon will discuss appropriate options and safety considerations.
When can I shower after surgery?
This depends on incision type, dressings, and your surgeon’s instructions. You will receive written guidance before discharge. Submerging incisions (bath/pool/ocean) is usually restricted for a period.
Safety & Credentials
Is the surgeon board-certified?
You should confirm your surgeon’s qualifications, scope of practice, and AHPRA registration. We encourage you to review AHPRA registration details and ask questions during consultation.
Where will the surgery be performed? Is the facility accredited?
Surgery is performed in an appropriate licensed surgical facility or hospital setting. Details of the facility and aftercare arrangements will be discussed during consultation.
Important Safety Information
Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
