Varicose Veins
Varicose vein treatment options in Sydney for symptoms and vein disease assessment
Overview
Add volume to breasts
Reduce sagging
Lift and tighten
Reshape and contour
Before & After
The outcomes shown are only relevant for this patient and do not necessarily reflect the results other patients may experience, as results may vary due to many factors including the individual’s genetics, diet and exercise.
Breast Augmentation
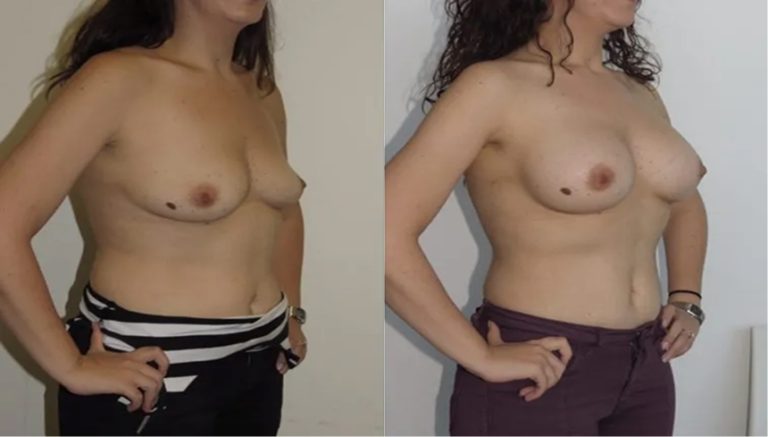
Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation
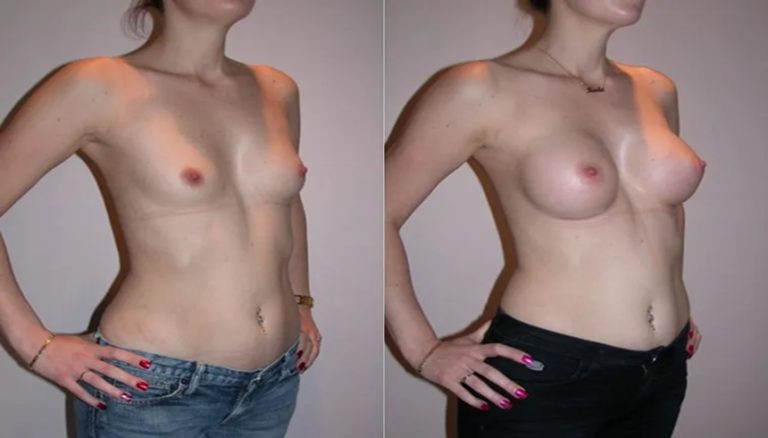
Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
About This Procedure
Your Consultation with Dr Lajevardi
Dr Sepehr Lajevardi is a highly skilled and experienced plastic surgeon, dedicated to providing exceptional results to each patient. He takes a caring approach, working with patients to create an individualised treatment plan that helps them feel confident in their outcomes. Book your appointment to receive professional care and guidance from Dr Lajevardi, and find out if breast augmentation surgery is right for you.

Key Benefits
Complete Vein Guide
Ideal Candidate
- Has varicose veins confirmed on assessment and appropriate investigations.
- Is medically suitable for the recommended intervention.
- Understands that outcomes vary and may require staged care.
You May Be a Good Candidate If
You may be a good candidate if you:
- You have symptoms or visible varicose veins and want an assessment.
- You can follow compression and aftercare instructions if advised.
- You understand treatment may involve multiple steps.
Who Should Not Undergo This Procedure
This procedure/treatment may not be appropriate if you:
- Pregnancy (some treatments are commonly deferred).
- Uncontrolled medical conditions that increase procedural risk.
- Expectation of guaranteed results or permanent prevention of recurrence.
Surgical Techniques & Approaches
Technique selection is individual and based on your anatomy, goals and safety considerations. Options may include:
- Ultrasound assessment: often used to map veins and identify reflux.
- Endovenous treatments (selected cases): thermal or non‑thermal ablation techniques may be considered.
- Sclerotherapy (selected cases): may be used for suitable veins or residual veins after other treatments.
- Surgery (selected cases): may be recommended depending on anatomy and severity.
Techniques & Approaches
Anesthesia
Pre-Operative Preparation
- Medical history and medication review, including clotting history.
- Bring compression stockings if advised.
- Follow fasting instructions if a procedure under sedation/general anaesthesia is planned.
Recovery Process
Timeline
Activity & Expectations
First Week
Weeks 2–6
3–6+ Months
Recovery Milestones
Return to Work
Return to Exercise
Assessing outcome
Resources & Guides
A breast augmentation is a very customized procedure, and selecting an experienced surgeon is paramount. Dr. Lajevardi focuses on patient safety, naturally appearing results, and transparency throughout the process.
Patient Preparation Guide
Procedure Walkthroughs

Procedure Walkthroughs


