Gender Affirmation Surgery (Bottom Surgery)
Overview
Gender affirmation “bottom surgery” refers to a range of genital reconstructive procedures that can modify external and/or internal genital anatomy in line with an individual’s goals as part of gender affirmation care. These are complex procedures that require careful assessment, detailed consent, and planned follow-up. A consultation is required to confirm suitability, discuss options and alternatives, and explain risks, scarring, and recovery. Outcomes vary and depend on anatomy, chosen technique, healing response, and post-operative care.
Add volume to breasts
Reduce sagging
Lift and tighten
Reshape and contour
Before & After
The outcomes shown are only relevant for this patient and do not necessarily reflect the results other patients may experience, as results may vary due to many factors including the individual’s genetics, diet and exercise.
Breast Augmentation
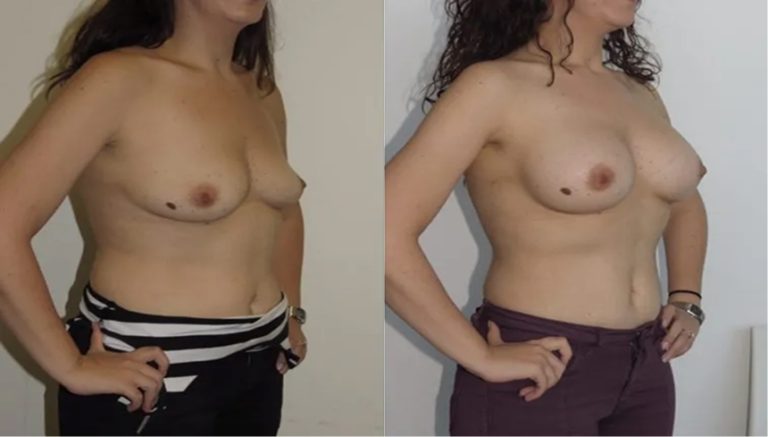
Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation
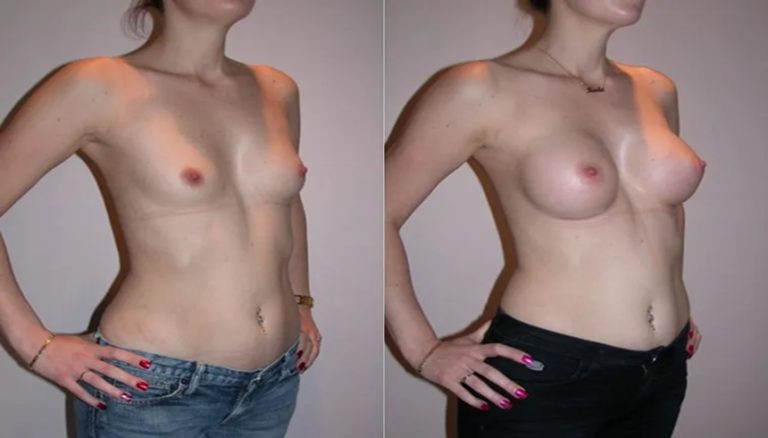
Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
Breast Augmentation

Implant Size: 300cc – 450cc
Recovery Timeline: 1–2 weeks light
Tags: Breast Enhancement, Cosmetic Surgery
About This Procedure
Bottom surgery is not one single operation. The most appropriate procedure (or staged plan) depends on anatomy, goals, health factors, and what is clinically suitable. Procedures are commonly discussed in two broad groups:
Male to Female (MTF) Procedures (selected cases)
These procedures may involve removal of testes and reconstruction of genital tissues to create external genital appearance and/or a vaginal canal, depending on the procedure selected.
Options that may be considered include:
Your Consultation with Dr Lajevardi
Dr Sepehr Lajevardi is a highly skilled and experienced plastic surgeon, dedicated to providing exceptional results to each patient. He takes a caring approach, working with patients to create an individualised treatment plan that helps them feel confident in their outcomes. Book your appointment to receive professional care and guidance from Dr Lajevardi, and find out if breast augmentation surgery is right for you.

- Orchidectomy (selected cases): removal of the testes. This may be performed as a standalone procedure or as part of a broader surgical plan.
- Vaginoplasty (selected cases): creation of a vaginal canal and external genital structures using established reconstructive techniques. Technique selection depends on anatomy and clinical factors.
- Vulvoplasty / “zero-depth” vaginoplasty (selected cases): creation of external genital structures without creating a vaginal canal.
- Labiaplasty / refinement procedures (selected cases): staged refinement of external tissues may be considered as part of the overall plan.
Female to Male (FTM) Procedures (selected cases)
These procedures may involve creation of a phallus or modification of existing genital tissues depending on individual goals and what is clinically suitable. Options that may be considered include:
- Metoidioplasty (selected cases): modification of the hormonally enlarged clitoris; may be combined with additional procedures depending on goals (e.g., urethral lengthening in selected cases).
- Phalloplasty (selected cases): construction of a phallus using tissue from a donor site (often performed in stages). Technique and staging depend on anatomy, donor site suitability, and clinical planning.
Key Benefits
The goal of a brow lift is to address specific structural features identified at assessment. Potential physical changes may include:
Reduction of upper‑lid hooding contributed to by brow position (where relevant).
Change in forehead contour and soft tissue drape (individual variation applies).
Symmetry cannot be guaranteed, and outcomes vary with anatomy and healing.
Complete Transgender Guide
Ideal Candidate
A suitable candidate is generally a healthy adult who has concerns related to brow position or forehead tissue laxity, understands that outcomes vary, and is comfortable with the presence of scars and recovery time.
You May Be a Good Candidate If
- You have brow position concerns that are not adequately addressed by non‑surgical options.
- You would like assessment for brow position and upper‑face changes.
- You understand that scars are permanent and vary in appearance.
- You can take time for recovery and attend follow‑up appointments.
- You do not smoke or can cease nicotine use as directed.
Who Should Not Undergo This Procedure
This procedure/treatment may not be appropriate if you:
- Uncontrolled medical conditions increasing risk.
- Inability to stop nicotine use when required.
- Expectation of a scar‑free or guaranteed outcome.
Surgical Techniques & Approaches
Bottom surgery uses reconstructive plastic surgery principles and may involve different approaches depending on procedure type and individual anatomy.
- Reconstructive tissue design and grafting (selected cases): skin grafts and/or tissue flaps may be used. Donor sites (where tissue is taken) will also heal and will scar.
- Microsurgery (selected cases): for some phalloplasty techniques, vessels and nerves may be connected using microsurgical methods to support tissue viability and potential sensory outcomes.
- Nerve preservation strategies (selected cases): where clinically appropriate, techniques aim to preserve key nerves; however, sensory outcomes vary and cannot be guaranteed.
- Urethral reconstruction (selected cases): may be required depending on the chosen procedure and goals. This can carry specific risks that will be discussed.
Anaesthetic
Genital reconstruction procedures are generally performed under general anaesthesia in an appropriately accredited hospital facility. Procedure duration varies significantly depending on the type and stage of surgery. Anaesthetic and hospital requirements are confirmed after clinical assessment and surgical planning.
Suitability
Suitability is determined during consultation and may involve coordination with your usual treating team. Factors commonly considered include:
- General health and medical stability for major surgery
- Ability to safely undergo general anaesthesia
- Understanding of the procedure plan, limitations, scarring, risks, and recovery demands
- Capacity to commit to post-operative care and follow-up (including dilation protocols for canal-forming vaginoplasty, where relevant)
- Smoking/nicotine status (nicotine can significantly increase complication risk)
Some patients may be advised to delay surgery to optimise health factors (e.g., smoking cessation, medical conditions, weight stability) or to complete required preparation steps.
Expected Scarring & Incisions
All surgery results in scarring. Scar location and visibility depend on the procedure, technique, and whether donor sites are used.
Examples of scar locations may include:
- Genital region incisions (procedure-dependent)
- Donor site scars (e.g., forearm/thigh for some phalloplasty techniques, where applicable)
Scars are permanent but typically change over time. Scar quality varies between individuals and can be influenced by healing response, infection, tension on wounds, and aftercare.
Risks & Considerations
All surgical procedures carry risks and outcomes vary. Your surgeon will discuss risks specific to your procedure plan and health profile. Potential risks may include:
- Bleeding, bruising, infection, delayed wound healing
- Scarring concerns (including hypertrophic scarring in some individuals)
- Adverse reaction to anaesthesia
- Tissue loss/compromised tissue viability (risk varies by technique, higher with nicotine use and some flap procedures)
- Urinary complications (e.g., strictures or fistulas), particularly where urethral reconstruction/lengthening is performed
- Sensory changes (temporary or permanent); sensation and sexual function vary and cannot be guaranteed
- Asymmetry, contour irregularities, or functional concerns requiring revision surgery (sometimes required, not guaranteed)
- Need for staged procedures and prolonged recovery depending on the surgical pathway
Your surgeon will also discuss procedure-specific considerations such as dilation requirements (for canal-forming vaginoplasty) and catheter care where applicable.
Recovery & Aftercare
Recovery varies by procedure type and staging. Hospital stay, catheter duration, wound care, activity restrictions, and time off work differ significantly between patients and procedures.
Examples of recovery considerations include:
- Hospital stay: varies depending on procedure complexity and individual needs
- Catheter care: may be required for a period after surgery (timeframe varies)
- Dilation protocols (selected cases): canal-forming vaginoplasty requires an ongoing dilation schedule; adherence is important and long-term maintenance may be required
- Return to work and exercise: depends on your procedure and healing; your surgeon will advise staged return to activity
Fees & Inclusions
Costs are highly individualised and depend on:
- The procedures selected and whether surgery is staged
- Hospital and anaesthetist fees
- Assistant surgeon fees (where required)
- Donor site requirements and complexity
A detailed written quote and financial consent are provided after consultation once a surgical plan is confirmed. Medicare and private health insurance arrangements vary based on item numbers and clinical indications and will be discussed with you.
Resources & Guides
A breast augmentation is a very customized procedure, and selecting an experienced surgeon is paramount. Dr. Lajevardi focuses on patient safety, naturally appearing results, and transparency throughout the process.
Patient Preparation Guide

Procedure Walkthroughs

Procedure Walkthroughs

Patient Preparation Guide
Frequently Asked Questions
Do I need a referral?
If you are seeking Medicare rebates for consultation or surgery (where applicable), a valid referral may be required. Our team can advise what is needed when you enquire.
Is sensation guaranteed after bottom surgery?
No. Techniques may aim to preserve nerves where clinically appropriate, but sensory outcomes vary between individuals and procedures and cannot be guaranteed.
What is the difference between vaginoplasty and vulvoplasty?
In general terms, vaginoplasty refers to procedures that create a vaginal canal (with ongoing dilation requirements), while vulvoplasty typically refers to creation of external genital structures without a canal. Suitability and implications are discussed during consultation.
Can bottom surgery affect urinary function?
Yes. These procedures may involve changes to the urethra depending on the technique. Urinary complications are possible and will be discussed as part of informed consent.
Important Safety Information
Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner. A consultation is required to determine suitability, explain risks and recovery, and discuss alternatives.
About the Specialist
Dr Sepehr Lajevardi (AHPRA: MED0001602957)
Registered Medical Practitioner – Specialist Plastic Surgeon (Specialist Registration in Surgery – Plastic Surgery). Procedure selection, staging, risks, realistic outcomes, and aftercare requirements are discussed in detail during consultation.

